The NHS Bed Management Playbook
The definitive operational guide for NHS leaders ready to reclaim lost capacity, reduce A&E boarding, and transform bed management from reactive chaos to proactive orchestration.
14,000
excess deaths/yr from A&E waits
13%
of beds blocked by delayed discharge
£37bn
capital investment shortfall
The State of NHS Bed Management
A System in Crisis
Data from the 2024 Darzi Report, BMJ Open, and NHS Operational Productivity reviews paint a stark picture.
0+
Excess Deaths Per Year
From A&E long waits
0K
Healthcare-Associated Infections
Annually in NHS England
0.0M
Bed Days Lost
To hospital infections alone
£0.0bn
Annual Cost of HCAIs
BMJ Open 2020 study
0.0M
Economically Inactive
Due to long-term sickness
£0bn
Capital Investment Shortfall
vs peer countries
0%
Beds Blocked
By delayed discharge patients
0%
A&E 4hr Performance
Down from 94% in 2010
Chapter 01
The Hidden Cost of Bed Mismanagement
Why the NHS loses 20-30% of bed capacity to coordination failures
"Patients no longer flow through hospitals as they should. Clinicians' efforts are wasted on solving process problems, such as ringing around wards desperately trying to find available beds."
- Lord Darzi Independent Investigation of the NHS, September 2024
Most NHS Trusts believe they operate at 90–95% bed occupancy. But the Darzi Report reveals a different story: effective utilisation - accounting for coordination delays, misplaced patients, and blocked beds - is 15–25% lower than reported. This "hidden capacity" represents thousands of available bed-hours lost every week to operational friction, not genuine demand.
The 2024 Darzi Report found that 13% of all NHS beds are occupied by patients waiting for social care support or care in more appropriate settings. Meanwhile, hospitals have seen a 17% rise in staff numbers since 2019, yet productivity has fallen - with 7% fewer daily outpatient appointments per consultant and 12% less surgical activity per surgeon.
A&E 4-Hour Target Performance Over Time
Source: Lord Darzi Independent Investigation 2024, NHS England
£11.6 billion
Backlog maintenance bill - hospitals disrupted 13 times per day in 2022-23
Lord Darzi Investigation 2024
300,000+ patients
Waiting over 12 months for treatment - 15x more than in 2010
Lord Darzi Investigation 2024

A&E departments across England now routinely see waiting areas at three times the patient volume they were designed for - a direct consequence of bed pressures upstream.
📷 Unsplash / National Health Service
- Whiteboards & phone calls for bed status
- 20-40 min delays per bed turn via bleeps
- No real-time visibility of hospital-wide capacity
- Reactive placement - wait for bed, then fill it
- No structured waiting list or placement preferences
- 13% of beds blocked by patients awaiting social care
- Real-time bed infographic - 7 statuses at a glance
- Intelligent placement helpers match patient to bed
- Hospital-wide dashboards for occupancy & capacity
- Structured waiting list with priority & preferences
- Full audit trail for every placement decision
- Role-based access - ward nurse to exec views
"If you had arrived at a typical A&E on a typical evening in 2009, there would have been just under 40 people ahead of you in the queue. By 2024, that had swelled to more than 100 people."
- Lord Darzi Investigation - Chapter 13
Chapter 02
What Top-Performing Trusts Do Differently
Lessons from the 15% of trusts achieving consistent flow

Top-performing trusts treat bed management as a clinical discipline. Their bed managers and site teams operate from real-time dashboards, not whiteboards or spreadsheets.
📷 Unsplash
The highest-performing NHS Trusts don't treat bed management as an administrative task - they treat it as a clinical discipline. They've moved beyond reactive bed allocation (waiting for a bed to become empty, then filling it) to proactive bed orchestration: predicting demand, pre-positioning capacity, and coordinating discharges hours before they happen.
35%
Bed-Turn Reduction
35-45 min faster
40%
A&E Boarding
40% fewer hours
25%
Elective Throughput
25% more procedures
18%
Overtime Costs
18% reduction
Real-Time Visibility as Standard
Every top-performing trust invested in real-time bed status visibility - not dashboards refreshed every 4 hours, but live, ward-by-ward views of bed state (occupied, pending discharge, being cleaned, available) accessible to bed managers, site coordinators, and ward leads simultaneously. This single change typically reduces bed-turn time by 35–45 minutes per patient.
Structured Discharge Rhythms
Instead of ad-hoc discharges, leading trusts implemented structured rhythms: morning board rounds at 08:00 with estimated discharge dates, "golden patient" identification (first discharge by 10:00), and afternoon validation rounds. This predictable cadence allows bed managers to forward-plan allocations rather than react to surprise discharges.
One NHS Trust transformed their clinical site team from a reactive model ("chaotic - feels like everyone making decisions about beds") to a proactive Flow Controller model with clearly defined roles:
Source: Clinical Site Team and On-Call Management - NHS Operational Guidance
Chapter 03
The Bed Flow Blueprint
A step-by-step framework for operational transformation
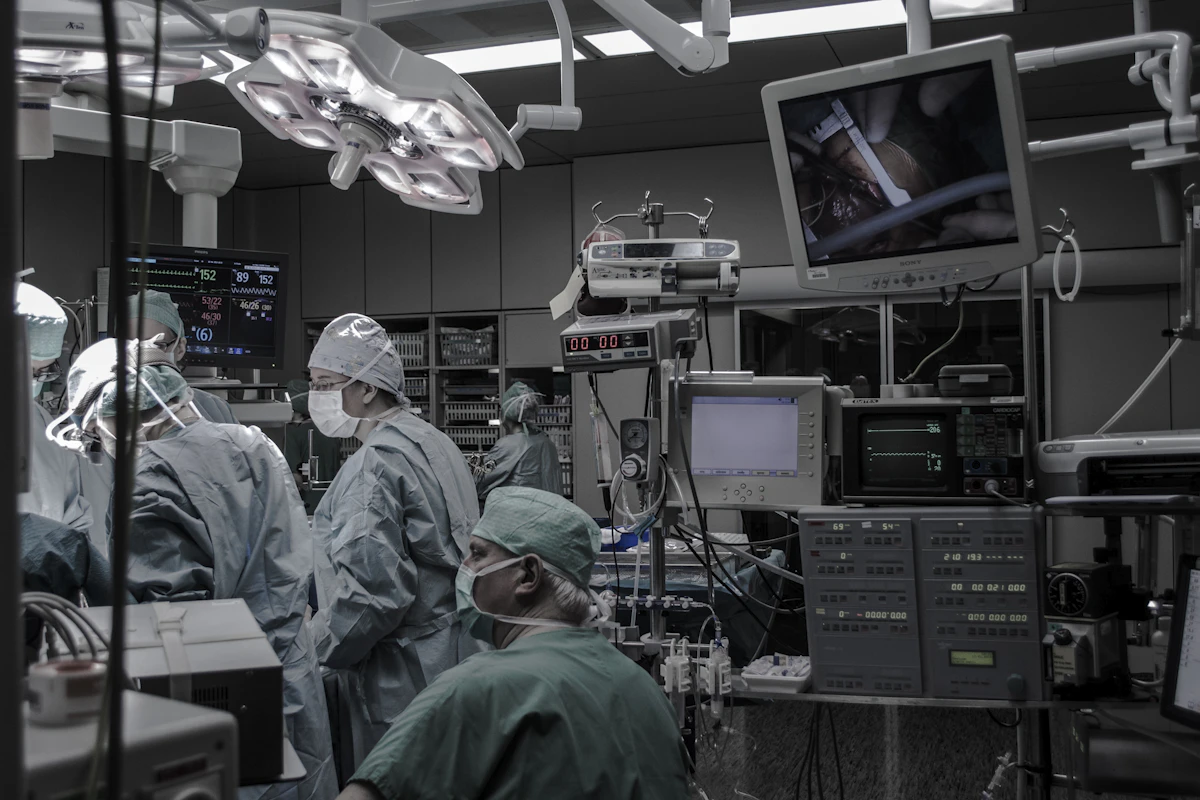
Flow transformation starts with a single ward. Trusts that achieve the greatest gains begin with a high-turnover pilot ward, build confidence among staff, then scale systematically.
📷 Unsplash
The Darzi Report is clear: "Drive productivity in hospitals... by fixing flow through better operational management, capital investment, and re-engaging staff." The Bed Flow Blueprint provides a practical, phased approach to achieving this - from establishing visibility to deploying intelligent orchestration.
See the Whole Picture
Place Smarter, Not Harder
Orchestrate, Don't Allocate
Want to see the Bed Flow Blueprint in action?
Book a strategic demo to see how inBedded implements each phase - real-time dashboards, placement helpers, and waiting list management.
Book a Strategic DemoChapter 04
Technology Selection Criteria
What to look for (and what to avoid) in bed management technology
"The NHS is in the foothills of digital transformation. The last decade was a missed opportunity to embrace the technologies that would enable a shift from 'diagnose and treat' to 'predict and prevent'."
- Lord Darzi Investigation 2024
Must-Have Capabilities
- Real-time updates with sub-60s latency
- Role-based views (ward nurse vs exec)
- Mobile-first - bed managers are mobile
- HL7/FHIR integration with PAS & EPR
- Architecture aligned with DSPT, DCB0129 & ISO 27001
Red Flags to Avoid
- Constant manual data entry with no automation
- One-size-fits-all - can't configure to your wards
- Legacy systems disguised as "digital"
- No placement logic or waiting list management
- Systems built without clinical risk management (DCB0129) principles

inBedded puts real-time bed visibility directly in the hands of nurses, bed managers, and site coordinators - on any device, anywhere in the hospital.
📷 Unsplash
Real-Time Bed Infographic
7 live statuses - Available, Occupied, Cleaning, Needs Cleaning, Hold, Pending Discharge, Out of Service
Intelligent Placement Helpers
Cosmas matching engine with 4 sensitivity levels (Low → Ideal) matching patients to beds by ward, type, gender & equipment
Waiting List Management
Priority-based queue with per-patient placement preferences - ward, bed type, and equipment configuration
Comprehensive Audit Trails
Full history of every patient placement, transfer, discharge, and bed status change - personal and ward-level
Real-Time Dashboards
Occupancy rates, available beds, cleaning status, COVID tracking, critical capacity alerts - all live
Role-Based Access
Ward-restricted views for nurses, Trust-wide visibility for site managers and executives
Chapter 05
12-Week Implementation Roadmap
From pilot to Trust-wide deployment
Implementation Timeline - Week-by-Week Progress
Discovery
- Map ward structure & bed types in inBedded
- Configure bed categories (Male/Female/Isolation/Unisex)
- Identify pilot ward (high-turnover)
- Train champion team (2-hour sessions)
Pilot & Iterate
- Go-live with dedicated support
- Enable Cosmas placement matching
- Activate waiting list & audit logs
- Target: 20% bed-turn time reduction
Scale Trust-Wide
- Expand ward by ward
- Enable cross-ward real-time dashboards
- Roll out RBAC for all staff tiers
- Begin quarterly impact reviews
Chapter 06
Measuring Impact
The KPIs that matter and how to track them
| KPI | Current Avg | Target | Improvement |
|---|---|---|---|
| Bed-Turn Time | ~180 min avg | < 90 min | 50% reduction |
| Discharge Before Noon | ~18% avg | 35%+ | 2x improvement |
| Elective Cancellation | ~8% avg | < 2% | 75% reduction |
| A&E to Ward Bed | ~5.2 hours avg | < 2 hours | 60% faster |
Return on Investment
£0.0M – £0.0M
Annual cost avoidance for a typical 500-bed trust. Return on Investment (ROI) typically realised within 4–6 months of full deployment.
Sources & References
- • Lord Darzi - Independent Investigation of the NHS in England, September 2024
- • Guest JF et al. - Modelling the annual NHS costs and outcomes attributable to HCAIs, BMJ Open 2020
- • NHS Improvement - Improving Patient Flow (ILG 2.3)
- • Lord Carter - Operational Productivity and Performance in English NHS Acute Hospitals
- • NHS England - Clinical Site Team and On-Call Management Guidance
- • The King's Fund - NHS 70: What will new technology mean for the NHS and its patients?
Ready to Transform Your Bed Management?
inBedded implements every framework in this playbook - real-time bed tracking, intelligent placement helpers, waiting list management, and comprehensive audit trails. See it with your Trust's data.
40%
less A&E boarding
25%
more elective cases
4-6
month Return on Investment (ROI) payback
Important Legal Notice: The NHS Bed Management Playbook is provided for educational and illustrative purposes only. While every effort has been made to ensure the accuracy of the citations (derived from the Darzi Report, Carter Review, BMJ Open, and NHS operational guidance), this document does not constitute formal clinical, financial, or operational advice.
AI Transparency: The synthesis, formatting, and drafting of this report may have been facilitated by artificial intelligence to ensure clarity and accessibility. The underlying data, statistics, and references remain entirely rooted in factual, publicly available healthcare literature.